10.22.25

Lumbar Injections Explained: How They Relieve Chronic Pain
08.29.25
PRP vs Steroid Injections: Which Is Better for Chronic Joint Pain?
07.25.25
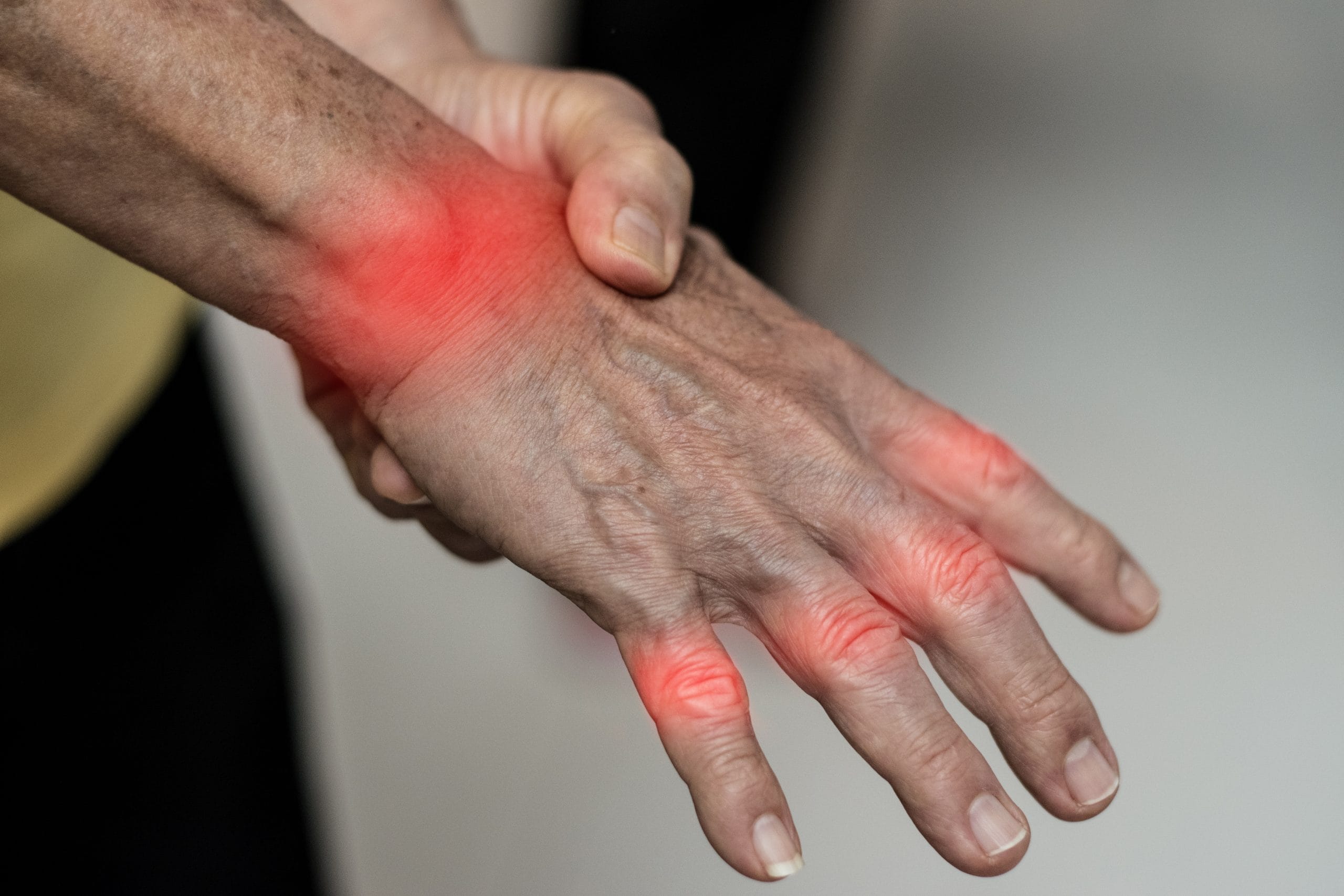
Effective Pain Management Solutions for Arthritis Sufferers
06.27.25

How to Manage Herniated Disk Pain Without Surgery
05.08.25

7 Signs You Need a Cervical Radiculopathy Specialist
04.30.25

Managing Fibromyalgia Pain: Treatments That Work
04.25.25
Living with Osteoarthritis? Discover Proven Treatments That Work
04.10.25
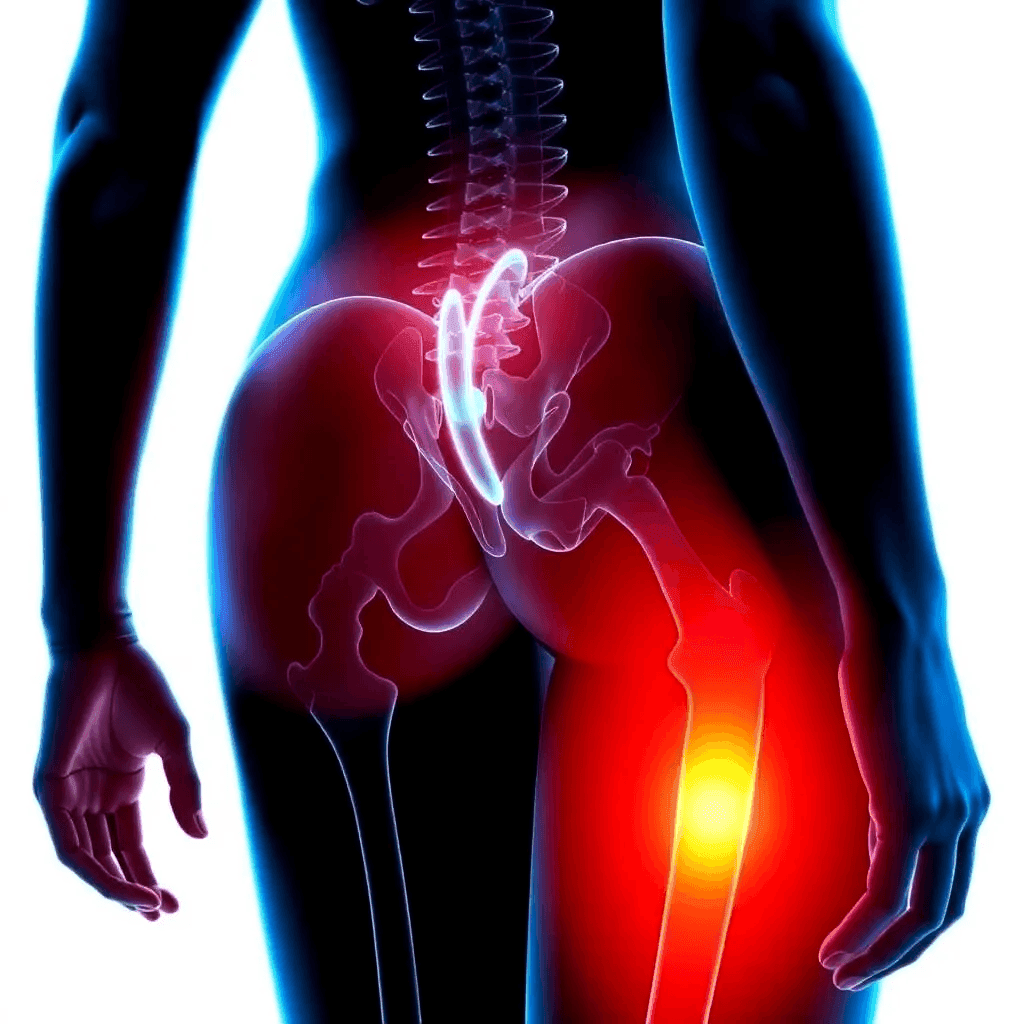
Sciatica Treatment Specialist in NJ – Find Lasting Relief with Dr. Todd Koppel

